
True Care’s medical billing services deliver structured, end-to-end support that helps healthcare providers turn clinical information into clean, billable insurance claims. By leveraging electronic billing systems and well-organized workflows, providers can accurately document diagnoses, procedures, and charges, then submit them to payers with confidence.
Beyond claim generation, our services also include comprehensive physician account management and medical billing administration. This covers patient claim invoicing, denial and rejection resolution, monitoring outstanding balances, and generating financial reports—helping practices strengthen revenue cycle performance and make better financial decisions.
Key components of our medical billing services include:
Expert patient billers offer the most complete medical billing services that entail handling check-in/out, claims, payments, and denials for health care providers.
Clinical coding officers translate patient services into ICD-10 and CPT codes and generate a clean “super-bill” for the biller to submit to the insurance payer.
Provider enrollment services by our credentialing specialists help healthcare providers join the network of desirable payors with maximum privileges.
Revenue cycle management services are specialty-specific, which means a physician’s bespoke demands are met by a dedicated medical biller.

True Care is a specialized medical billing partner dedicated to accurate and efficient medical claims processing.
Managing billing claims can be challenging for providers who aim for timely submissions and complete reimbursement for the care they deliver—but with True Care’s focused medical billing solutions, the process becomes seamless and stress-free.
We streamline every stage of the billing cycle, combining strong clinical expertise with a commitment to high-quality claims handling. Using secure cloud-based technology, we instantly verify patient insurance eligibility and submit claims electronically to accelerate payments. In addition, our experienced billing professionals ensure that every claim is properly processed and reaches the insurer, maximizing reimbursements for healthcare providers.
When “good enough” isn’t enough, you need a specialized medical billing agency.
As a leading medical billing services provider, our billing firm wrings every last dollar from a provider’s claims via 24/7 billing cycle oversight. We’re experts on the big commercial ones, Aetna and Blue Cross Blue Shield. We know the government plans inside and out, Medicare and Medicaid.
We work hand in glove with the top payers so the provider billing reimbursement forms like CMS-1500, CMS-1450 (UB-04), and CMS-1728-20 are shipshape. True Care RCM medical transcription and billing company makes claims and repayments happen, period!
With a 4.8-star Trustpilot rating from more than 200 reviews, a 4.8-star Google rating from 340+ reviews, and an A+ rating from the Better Business Bureau, True Care RCM is widely recognized as one of the best medical billing service providers in the United States.

Over 1500 medical practices trust True Care RCM medical billing services company. So let’s have a chat.

Traditional agencies have a 50% failure rate with provider credentialing and patient billing.
True Care achieves a 97% clean-claim acceptance rate and also provides dedicated support to review, correct, and resubmit denied claims efficiently.
Save over in-house billing with our affordable 2.49% collections rate, pay-for-paid model, free EMR software, scalability, and free denied claims appeals. Outsource to us for billing optimization with complimentary perks like:
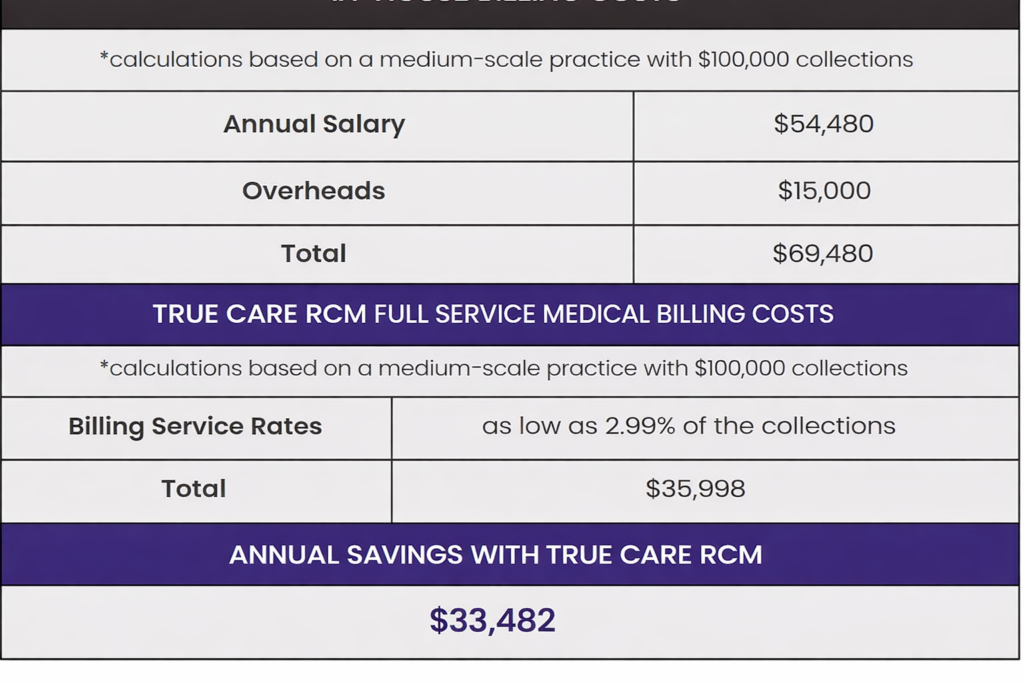



For a medical practice, medical billing services handle the logistical details of getting paid by insurance companies and patients. Billers take over the coding, filing, follow-up, and payment posting for claims. They have the latest knowledge and technology to optimize the process. Healthcare providers benefit through reduced costs, improved cash flow, decreased claim denials, and the ability to focus on patients, not accounts and invoices.
Medical billing services manage every financial touchpoint after a patient visit: verifying coverage, coding procedures, filing claims, appealing denials, and depositing funds to ensure healthcare providers receive full, compliant reimbursement.
Our medical billing firm offers a range of services, such as provider enrollment, insurance verification, charge entry, claim submission, payment posting, account receivable management, denial management, appeal management, patient billing, reimbursement tracking, and collection
Accurate claim submission is only the beginning. We take over from there, communicating with payers to shepherd each claim to resolution. Tracking status closely allows rapid response to any issues. Underpayments and denials receive dogged follow-up and appeal when justified. Years of experience equip us to overcome obstacles and ensure you receive every dollar, on time. Claims reimbursement is complex but our expertise delivers results.
Of course. True Care RCM lets providers track the caliber and results of their facility’s billing. We also share reports on daily invoicing, key markers and offer feedback for revenue cycle advancement.
